General verification
This chapter describes what verification is required and when.
-
WAC 182-503-0050 Verification of eligibility factors.
-
WAC 182-503-0050 Verification of eligibility factors.
Effective November 3, 2019
- General rules.
- We may verify the information we use to determine, redetermine, or terminate your apple health eligibility.
- We verify the eligibility factors listed in WAC 182-503-0505(3).
- Before we ask you to provide records to verify an eligibility factor, we use information available from state databases, including data from the department of social and health services and the department of employment security, federal databases, or commercially available databases to verify the eligibility factor.
- We may require information from third parties, such as employers, landlords, and insurance companies, to verify an eligibility factor if the information we received:
- Cannot be verified through available data sources;
- Did not verify an eligibility factor; or
- Is contradictory, confusing, or outdated.
- We do not require you to submit a record unless it is necessary to determine or redetermine your eligibility.
- If you can obtain verification within three business days and we determine the verification is sufficient to confirm an eligibility factor, we base our initial eligibility decision upon that record.
- If we are unable to verify eligibility as described in (f) of this subsection, then we may consider third-party sources.
- If a fee is required to obtain a necessary record, we pay the fee directly to the holder of the record.
- We do not deny or delay your application if you failed to provide information to verify an eligibility factor in a particular type or form.
- Except for eligibility factors listed in WAC 182-503-0505 (3)(c) and (d), we accept alternative forms of verification. If you give us a reasonable explanation that confirms your eligibility, we may not require additional documentation.
- Once we verify an eligibility factor that will not change, we may not require additional verification. Examples include:
- U.S. citizenship;
- Family relationships by birth;
- Social Security numbers; and
- Dates of birth, death, marriage, dissolution of marriage, or legal separation.
- If we cannot verify your immigration status and you are otherwise eligible for Washington apple health, we approve coverage and give additional time as needed to verify your immigration status.
- Submission timelines.
- We allow at least ten calendar days for you to submit requested information.
- If you request more time to provide information, we allow the time requested.
- If the tenth day falls on a weekend or a legal holiday as described in RCW 1.16.050, the due date is the next business day.
- We do not deny or terminate your eligibility when we give you more time to provide information.
- If we do not receive your information by the due date, we make a determination based on all the information available.
- Notice requirements.
- When we need more information from you to determine your eligibility for apple health coverage, we send all notices according to the requirements of WAC 182-518-0015.
- If we cannot determine you are eligible, we send you a denial or termination notice including information on when we reconsider a denied application under WAC 182-503-0080.
- Equal access and limited-English proficiency services. If you are eligible for equal access services under WAC 182-503-0120 or limited-English proficiency services under WAC 182-503-0110, we provide legally sufficient support services.
- Eligibility factors for nonmodified adjusted gross income (MAGI)-based programs. If you apply for a non-MAGI program under WAC 182-503-0510(3), we verify the factors in WAC 182-503-0505(3). In addition, we verify:
- Household composition, if spousal or dependent deeming under chapter 182-512 WAC or spousal or dependent allowance under chapters 182-513 and 182-515 WAC applies;
- Income and income deductions;
- Resources, including:
- Trusts, annuities, life estates and promissory notes under chapter 182-516 WAC;
- Real property transactions; and
- Financial records, as defined in WAC 182-503-0055, held by financial institutions.
- Medical expenses required to meet any spenddown liability under WAC 182-519-0110;
- All post-eligibility deductions used to determine cost of care for clients eligible for long-term services and supports under chapters 182-513 and 182-515 WAC;
- Transfers of assets under chapter 182-513 WAC and WAC 182-503-0055 when the program is subject to transfer of assets limitations;
- Shelter costs for long-term care cases where spousal and dependent allowances apply;
- Blindness or disability, if you claim either; and
- Social Security number for a community spouse if needed when you apply for long-term care.
- Verification for MAGI-based programs.
- After we approve your coverage based on your self-attestation, we may conduct a post-eligibility review to verify your self-attested information.
- When conducting a post-eligibility review, we attempt to verify eligibility factors using your self-attested information available to us through state, federal, and commercially available data sources, or other third parties, before requiring you to provide information.
- You may be required to provide additional information if:
- We cannot verify an eligibility factor through other data sources listed in subsection (b) of this section; or
- The information received from the data source is not reasonably compatible with your self-attestation.
- Reapplication following post-eligibility review. If your eligibility for MAGI-based apple health terminates because of a post-eligibility review and you reapply, we may request verification of eligibility factors prior to determining eligibility.
This is a reprint of the official rule as published by the Office of the Code Reviser. If there are previous versions of this rule, they can be found using the Legislative Search page.
- General rules.
Worker responsibilities
Before requesting verification:
- Look in the case record (Washington Healthplanfinder document center, Barcode ECR, WebAx, case notes) and third party sources to verify the information.
- Only request verification needed to verify the eligibility factor.
- Do not request verification to be in a particular type or form. For instance, do not ask for a bank statement to verify resources. Instead, request "proof of resources, such as a bank statement for the month of March, 2023".
- Use alternative methods, such as telephone calls, as the primary method to verify the client's circumstances. Request paper verification only when there are no other methods readily available.
When verification is needed:
- Verification may be needed when the information received is questionable. Consider the information questionable when it:
- Contradicts or conflicts with other statements made by the client;
- Is received from a third-party source that contradicts or conflicts with other statements made by the client; or
- Calls into question the accuracy of the information provided by the client.
- Ask for documents the client can easily get. If it will take the client more than three business days to get the verification, such as immigration documents, offer to help get it. Do not deny or terminate Apple Health if the client is responding to verification requests by reporting they need more time.
- If the client has a disability or needs equal access services, offer to help get the information.
- If the verification will cost money (such as out-of-state birth, death, or marriage certificates, medical information, copies of bank statements, etc.), explore alternate verifications before offering to purchase the items.
Processing verification received:
- Accept reasonable explanations. Use the prudent person concept and document this.
- When a client provides partial verification, send another request letter asking for more information and allow more time. The exception is when the provided verification confirms the client is not eligible. For example: a worker requests proof of income and citizenship, but only receives the income verification. The income verification shows the client is over income. It is not necessary to re-pend for the citizenship verification. Apple Health can be terminated for over income.
- Use the following criteria to evaluate verification and verbal/written statements used for verification:
- Does it verify the eligibility factor? (For example, a child's birth certificate verifies age and citizenship, but not residency.)
- Is the document/statement the most reliable available evidence?
- Was the document/statement prepared near the time the event took place?
- Is the document/statement signed and dated?
- Has the time period the document/statement covers expired?
- Does the document appear to be altered?
- After evaluating a document on the above criteria, determine if you have enough information to establish eligibility. If not, document the reason and request further verification.
Certain eligibility factors do not change and do not require another check in the future, including:
- US citizenship (unless extremely rare circumstances);
- Family relationships by birth, marriage, and divorce; and
- Social Security Numbers (unless in the rare circumstance the client has more than one).
Documentation:
- When requiring additional verification, document why additional verification is needed.
- What to document for each case:
- What verification you requested;
- Why you requested verification/additional verification;
- What verification you received;
- When you received the verification;
- What action you took, if any, to help the client get the verification;
- Whether the client has a disability that would make it hard or impossible to get the verification, and/or whether the client is a victim of domestic violence and failed to get the verification due to the domestic violence;
- Whether the client has been designated as Equal Access (EA) and if so, whether you followed the EA Plan.
- What decision or action you took.
- In the letter to the client, explain what information was requested and that it was not received or explain it was received but did not verify eligibility.
Granting a reasonable opportunity period:
A ROP is granted when a client attests to a satisfactory citizenship or immigration status that is not verified using existing crossmatches. Before requesting verification:
-
- Look in the case record (Washington Healthplanfinder document center, Barcode ECR, Laserfiche, SAVE Verification in ACES, case notes) and third-party sources to verify the information and review for typos that may prevent verification.
- Send a notice requesting verification, with a due date of at least 10 days to provide verification.
- If verification has not been provided the client has the rest of the 90 days to provide verification and continues to receive Apple Health.
- When verification is received, use SAVE to verify the document and the client’s status. The client continues to receive Apple Health while a response from USCIS is received, which may exceed the initial 90-day ROP period.
- Update the application and case record to either approve or terminate coverage.
Verification of citizenship/identity for Classic Apple Health/non-MAGI and some MAGI-based cases can be found in ACES:
| Citizen valid value | identity valid value |
|---|---|
| T1, T2, EW or FV | V, E or F |
Individuals who match with the SSA interface for citizenship/identity will automatically be updated by ACES with "FV" valid value for citizenship and "F" valid value for identity.
If it is determined the interface is in error and the federally verified codes need to be changed, call or email:
Chris Stehr 360-725-1304 chris.stehr@hca.wa.gov
Rebecca Janeczko 360-725-1390 rebecca.janeczko@hca.wa.gov.
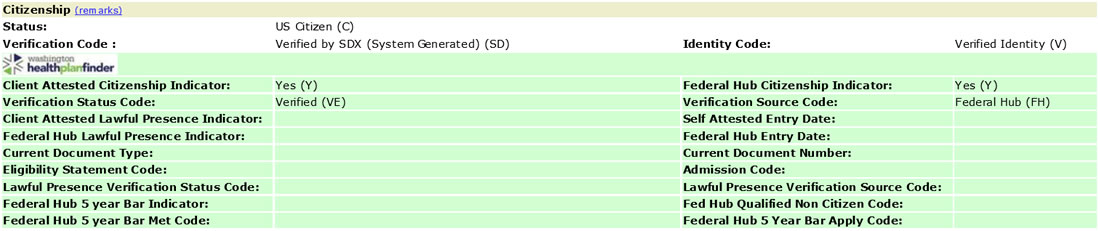
For MAGI-based Apple Health through Washington Healthplanfinder, citizenship and lawful presence is found in ACES Online on the Client >> Demographic screen.
Example of a client’s citizenship attestation that was verified through the federal hub:

Example of a client’s lawful presence attestation that was verified through the federal hub:
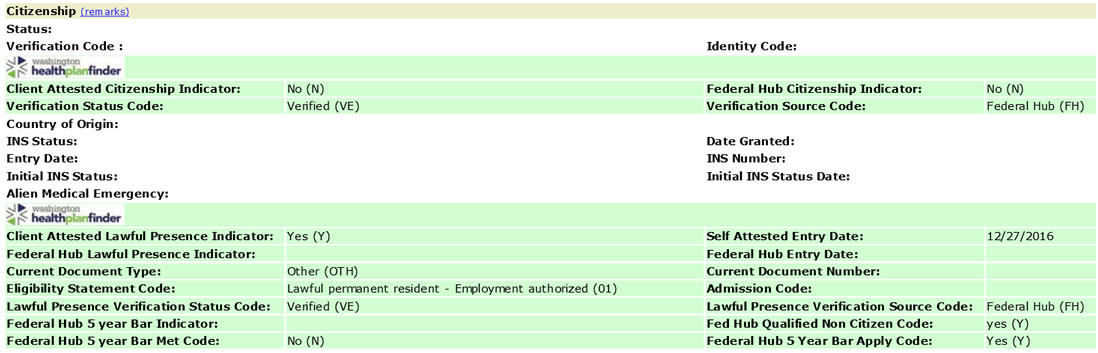
Survivors of domestic violence/ACP participants
If a client is a victim of domestic violence:
- Have the client write a statement that explains what proof or way of getting proof would put the client and/or children at risk of harm, if any.
- Help the client get proof that will not put them at risk.
- For a victim of domestic violence who is also an immigrant, consider a referral to an immigration attorney or to the Northwest Immigrant Rights Project.
Example: A woman and her two children apply for coverage. They are living at the local domestic violence shelter and the father of the children lives in the family home. Do not call the family home to verify any information. Do not require the victim to return to the home to get any verification.
When a client presents an ACP authorization card:
- Enter the ACP address into Healthplanfinder or ACES. Only call the ACP at 360-753-2972 to verify that the client is currently certified in the program if return mail is received.
- If the client is currently certified in the ACP:
- In Washington Healthplanfinder, enter PO Box 257. This triggers a popup to enter the post mail box (PMB). Enter the PMB and Olympia, WA 98507.
- In ACES, enter the ACP mailing address and participant code number as shown on the card in place of the client's physical address on the ACES ADDR screen.
- Mail all letters to the substitute address.
- Do not ask the client to provide their actual address. Do not record the client's physical address in any case notes or retain copies of any documents that list the client's physical address.
- If information is found or entered that could be used to locate an ACP client, notify your supervisor to redact information from ACES and/or Washington Healthplanfinder.
- When verifying residency, household composition, or shelter costs, do not ask the client to provide documents that state their physical address. Accept any document that lists the ACP address and reasonably verifies the eligibility factor.
- If the client provides a document that lists the physical address, work with a supervisor to contact ACES, Barcode and/or HPF to remove any reference to the address.

